Your claims get paid.
Just not enough.
Vareo catches every underpayment, in-network or out, and recovers what you're owed. End to end, on contingency.
Serving clients across every need
Insurance companies underpay you. Systematically.
Lost Every Year
Payers systematically underpay against contracted rates through fee schedule misapplication, modifier downcoding, and incorrect bundling.
Industry estimate based on commercial payer remittance analysis
Of Claims Underpaid
Nearly one in three claims is paid below the contracted rate. Without automated tools, most providers never catch them at scale.
Across commercial payer mix; varies by specialty and payer
Never Recovered
Timely filing limits turn underpayments into permanent losses. Every day you wait, more revenue becomes unrecoverable.
Per MGMA and HFMA: timely filing limits and limited internal recovery capacity
From connection to recovery. Three steps.
Connect Your Data
Bring your data however it moves. Clearinghouses, SFTP, encrypted email, file upload, PM system exports. We handle 835s, 837s, EOBs, and more. Setup takes under an hour.
AI Audits Every Claim
Vareo compares every payment against contracted rates, modifier rules, and payer-specific logic. Not a sample. Every claim, every time.
We Recover What's Yours
Vareo generates appeals, submits to payers, and follows up end to end. You pay nothing unless we put money back in your pocket.
The variances payers count on you missing. Caught.
Five categories of commercial payer underpayments that show up on every remittance file we've audited. Hover any tile for the contract math we use to flag it.
Fee Schedule Misapplication
Payer applies incorrect or outdated fee schedule rates.
Modifier Downcoding
Payer downcodes modifiers to reduce reimbursement.
Incorrect NCCI Bundling
Mutually exclusive procedures bundled when modifier 59 or XS/XE applies.
Contract Rate Errors
Wrong tier, wrong effective date, or wrong contract terms applied.
Invalid Filing Denials
Claims denied as "late" when submitted within deadline.
Plus the long tail.
Carve-out misapplication, multiple-procedure reductions, place-of-service downgrades, contract effective-date mismatches, and the dozens of payer-specific edge cases that only show up when you audit at the line-item level.
For groups where out-of-network is a meaningful share of revenue.
Hospital-based specialty groups in emergency medicine, anesthesia, radiology, and pathology live and die on out-of-network reimbursement. Vareo runs the full federal IDR workflow so you stop leaving QPA-anchored awards on the table.
Open Negotiation Tracking
Every open-negotiation period is tracked from the day the IDR clock starts. Counter-offers, deadlines, and payer response windows are managed in one place.
QPA Validation
Qualifying Payment Amounts are sanity-checked against your historical commercial median, the geographic norm, and the carrier’s public methodology. Anomalies are surfaced before you accept.
Stronger Cases, Higher Awards
Vareo learns from every public IDR decision and tailors each filing to the arguments and comparable rates that have historically won for your specialty and CPT mix. Better-built cases win more often, and at higher amounts.
Award Enforcement
When the IDRE rules in your favor, Vareo confirms the award is paid in full within the federal 30-day window. Late or partial payments trigger automatic enforcement escalation.
If your group is doing IDR by spreadsheet, it isn’t doing IDR.
Talk to us about NSAOpen Vareo. See your money.
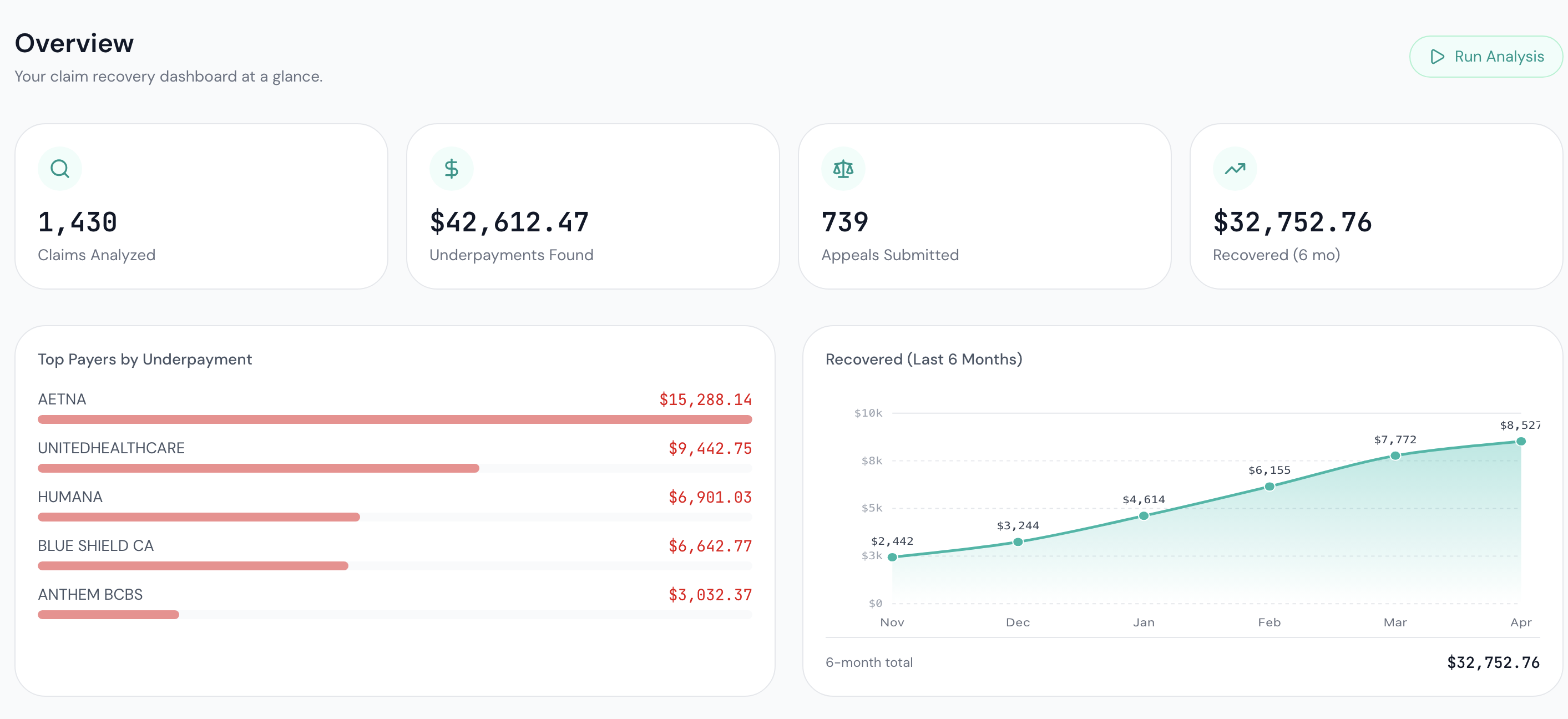
Your dashboard shows every recovered dollar, every active appeal, and every payer behavior pattern your practice should know about.
See exactly what we found and why. Every flagged underpayment is auditable down to the original claim, the contracted rate, and the variance. You can validate any recovery against the source data.
Know which payers cost you most. Recovery patterns by payer, by CPT code, by month. The same data Vareo uses to find variances is data your practice can use to renegotiate contracts at renewal.
Built for healthcare. Secured like it.
HIPAA Compliant
All data is encrypted at rest and in transit. Zero PHI exposure. Full audit trail on every interaction with your claims data.
ActiveBAA Available
We sign a Business Associate Agreement with every client before any PHI is exchanged. No exceptions, no workarounds. Standard practice.
StandardSee what you could be recovering.
Zero risk. You pay only
when we recover.
Contingency-based pricing means no setup fees, no monthly fees. We only get paid when you do. Book a free assessment to see your recovery potential.
Get Your Free Assessment